A STROKE OR NOT A STROKE?
Practicing medicine, every day is filled with solving “puzzles” one after another. These “puzzles” appear in your office in the form of a human being in whom some of the puzzle pieces are present but many are missing. The doctor sees some of the pieces, immediately, when the patient first appears in the exam room, but many pieces are hidden, and must be discovered by doing a thorough physical examination and special testing. Putting all “the pieces” together makes it possible to find the origin of the patient’s problem. When that is accomplished, the doctor now has all he needs to make a diagnosis and complete the puzzle.
One great example of this complex problem was shared in an article in medscape.com where they presented the case of a man with a violent cough, a droopy eyelid, slurred speech, and significant weakness in his left arm and leg. The man was 57 yo and was rolled into the exam room in a wheelchair. He complained of a cough he’d had for a week that was at times very “violent.” He was in a wheelchair because he was unable to use his left arm and leg and could not walk. The doctor also noted the upper eyelid of his right eye was drooping and his speech was slurred. His left eye was normal. So, the doctor was faced with the challenge to explain all of these varying symptoms and physical findings.
At first glance, it appears this man has had a stroke. His left sided extremity weakness is consistent with stroke, but a droopy right upper eyelid doesn’t fit. In the usual left-sided stroke, the right side of the brain is affected, but the physical findings are all on the left side of the body; including the face and eyes. A one-sided droopy upper eyelid is not part of the usual right-brain, left-side stroke. The pupil of his right eye is very constricted, also. His speech is slurred. There is a loud bruit (sound of turbulent blood flow) over the right carotid artery. The patient also has a cough described as violent. That means the cough was deep, dry, frequent, and very forceful. It’s the kind of cough that would make your face and neck very red. His heart and lungs exams were normal.
To evaluate his symptoms and physical findings, the following tests were done:
Chest X-ray—normal, no pneumonia, mass lesion, no fluid
Chest CT—normal, the cough may be viral or from another source
Head CT—abnormal: the right middle cerebral artery is hyperdense meaning it is
compromised by some insult. The RMCA is the main blood supply to the R brain.
If blood flow is impeded, the artery appears abnormal on CT. The brain tissue on
the right side did not appear damaged (infarcted).
Carotid Angiogram—the loud bruit over the right carotid and stroke-like findings on his left
side point to a problem with the right carotid artery. Angiography showed an
abrupt narrowing of the internal carotid consistent with a tear in the artery wall.
Summary of the case:
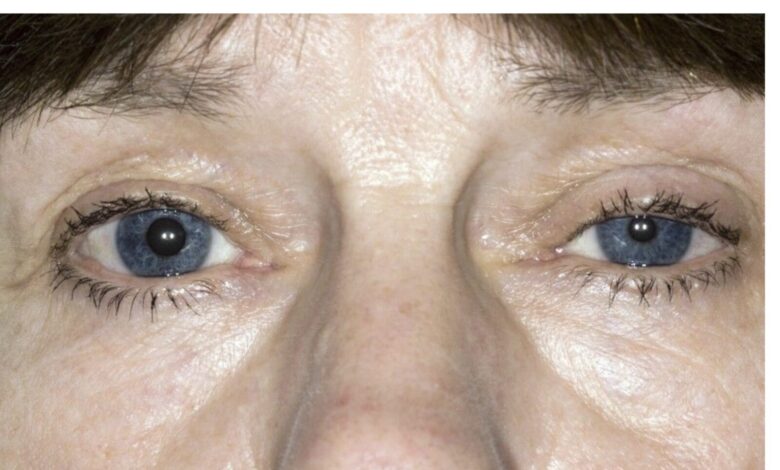
1. Right eye findings—the patient has Horner’s syndrome. This is the the triad of ptosis (drooping of the upper eyelid), miosis (constriction of the pupil), and decreased sweating on the affected (right side) of the face. Sometimes the affected eye will sink into the bony orbit (enophthalmos). Horner’s Syndrome is caused by disruption of the sympathetic nerve fibers that travel along the carotid artery to the eye and control pupillary dilation and constriction and blinking.
2. Carotid artery disruption—the loud bruit over the right carotid means something is wrong with the right carotid. Violent coughing has caused disruption of the inner lining of the right carotid artery. Blood forced its way through a tear in the artery’s inner lining and pushed its way between the layers of the carotid artery wall causing two problems: A. Damage to sympathetic nerves traveling with the carotid to the right eye causing Horner’s Syndrome. B. Plaque in the carotid artery wall ruptures, breaks loose, and flows up into the right middle cerebral artery occluding it causing left sided weakness.
3. Diagnosis: A. Traumatic dissection of right carotid artery
B. Right Horner’s syndrome
C. Right Middle Cerebral Artery Occlusion
D. Left-Sided weakness due to “C.”
This patient is not typical of the kind of problem you would see in the family doctor’s office. This problem is complex, requires blood tests and imaging studies, and is more suited to be evaluated in the ER. Had he been brought to my office, after evaluating his physical status, I would have called an ambulance and had him transported to the ER. He would almost certainly have been admitted to the hospital and then, evaluated and treated as an inpatient.
This man had arteriosclerosis of his carotid arteries. He developed a severe cough that increased the pressure within the carotids and tore a small hole in the inner lining of the right carotid. The pressure of the blood flowing through the carotid forced blood to flow between the layers of the artery wall (carotid dissection) damaging the sympathetic nerves and causing Horner’s Syndrome.
The right middle cerebral artery, the main source of blood to the right side of the brain, is clogged/occluded by fragments of arteriosclerotic plaque that have broken loose at the site of dissection and flowed upward into the artery blocking blood flow. Lack of blood means lack of oxygen to the brain and damage to the brain tissue causing left-sided stroke-like symptoms. So, this patient did have a stroke caused by an unusual problem. It happened all because of damage to the right carotid artery at the site of an arteriosclerotic plaque. That occurred because violent coughing increased the pressure within the carotid tearing a small hole in the lining.
This medical “puzzle” was indeed a challenge. The pieces aren’t always all there laid out in front of you to assemble logically. The doctor has to do tests to find those missing pieces so he can finish the “puzzle”/diagnosis. In this case, all the pieces were found and fit nicely into a logical diagnosis. Now, we have to hope that appropriate treatment will improve the problem and improve the patient’s condition.
Reference: Brillo F, Tomalleri G. Man with a Violent Cough Develops Ptosis and Slurred Speech Medscape 2025 Dec 15.
www.medscape.com/viewarticle/Man-violent-cough-develops-ptosis-slurred-speech