WHAT’S A MORTON’S NEUROMA?
Doctor’s like to name diseases, procedures, or body parts for themselves. Have you ever heard of Bright’s Disease, the Hartman procedure, or the Sphincter of Oddi? Probably not, but Doctors Bright, Hartman, and Oddi wanted other doctors to remember them when they read about kidney disease, diverticulitis, or gall stones. I don’t know if it’s an ego thing, but it probably is because I know physicians who have a lot of it. The general public sees examples of it every day.
Another example would be a doctor who undoubtedly saw a lot of patients with painful feet. Thomas George Morton (1835-1903) received his MD degree in 1856 from the University of Pennsylvania. He practiced general surgery and was head physician at Pennsylvania Hospital for years. He had extensive experience treating soldiers during the Civil War and founded many military hospitals. Dr. Morton was the first surgeon to successfully diagnose and remove an inflamed appendix. He was a prolific author writing on numerous medical subjects. But in 1876, his name was forever immortalized.
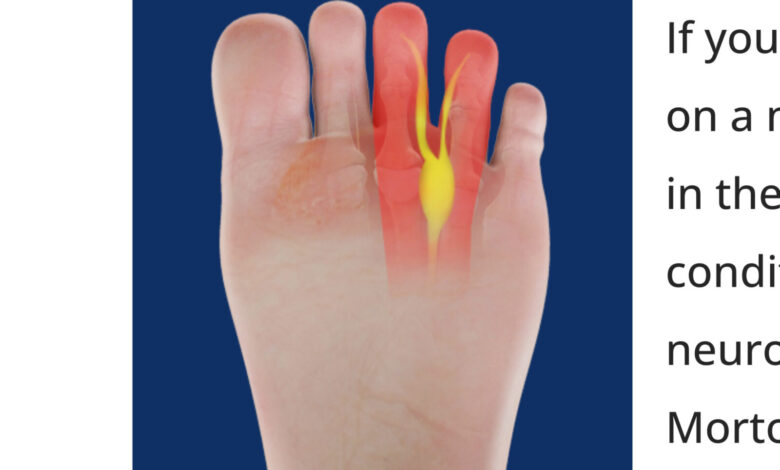
It was then he described 16 patients he had seen with “metatarsalgia.” At least that’s what he called the pain people described in their forefoot between their toes. One of these 16 patients had hurt her foot stepping on a rock four years earlier. He suspected the pain was from a injury to the head (end) of the 4th metatarsal so he surgically removed the end of the bone and the digital nerves on either side of the metatarsal. After recovering, she was pain free. The tissue Morton removed was closely analyzed, and it was determined the pain actually originated from the digital nerve running under the metatarsal head. Excising the metatarsal head was unnecessary. The nerve was entrapped by a metatarsal ligament and had degenerated and become scarred. A scarred, compressed nerve causes pain whenever it is compressed further.
Dr. Morton called his discovery Morton’s metatarsalgia, and later, Morton’s Neuroma, even though it was scar tissue and not a neuroma, per se. Patients describe the pain as “burning, stabbing, or tingling with electric sensations.” Morton’s neuromas occur in women five times more often than men, and there is predilection for them to occur between the third and fourth metatarsal heads. That space is narrower than the other inter-metatarsal spaces. The pain is aggravated by walking, direct pressure, or wearing tight-fitting, high-heeled shoes.
Conservative treatments include “wide, soft-soled, laced shoes with low heels….metatarsal pads….anti-inflammatory meds….gabapentin…..steroid (cortisone) injections…..radio frequency ablation, cryotherapy, and alcohol nerve injections.” But each of these provide only temporary relief. When conservative treatments fail, surgical excision of the “neuroma” is indicated. Most often, the incision is made between the metatarsals on the top of the foot, and the ligament impinging the nerve is “transected” (cut). The impinged portion of the nerve is excised, too. References cite success rates after surgery as “32% good” and “45% excellent.” Only “8% of patients report poor results.”
In the hands of a good podiatrist, surgery has a “100% success rate.” If the surgeon is able to identify the abnormal tissue, and remove it completely, the results are always good. I have also been informed that “sclerosing” the “neuroma” with a local injection of alcohol has been very effective as well. Of course, the doctor who injects the neuroma has to be on his/her game because efficacy is entirely dependent on the surgeon’s ability to find the lesion and inject it appropriately.
I diagnosed Morton’s Neuroma very infrequently, but I saw several patients who had had one, or more, surgically excised and were pleased with their results. Unfortunately, fairly often, patients will have a second neuroma, usually in the same foot, or if the neuroma is inadequately excised, it can reoccur. “The failure rate following surgical excision has been reported as up to 30%,” but when you cut a nerve, the exposed ends tend to scar and re-form neuromas.
The “take home message” for Morton’s neuromas is try non-surgical treatment first, but if it fails, surgery is indicated knowing the rate of “recurrence is very high.”
After reading about the many accomplishments of Dr. Thomas George Morton 150 years ago, when there were no electric lights, computers, and the telephone had just been invented, I have no business criticizing him for naming a foot condition for himself. In fact, the many things he accomplished, or was the first to do, relegate him to the higher echelon of individuals with incredible courage and genius.
References: https://jamanetwork.com/journals/jama/article-abstract/2812902
Bhatia M, Thomson L. Morton’s Neuroma—Current Concepts review. J Clin Orth Trauma 2020 Apr 10;11(292):406-409.
Mak MS, Chowdbury R, Johnson R. Morton’s Neuroma: review of anatomy, pathomechanism, and imaging. Clin Radiol 2021 Mar;76(3):235.
Thomson L, Aujia RS, Duvall P, Bhatia M. Non-Surgical Treatments for Morton’s Neuroma: A systematic review. Foot Ankle Surg 2020 Oct;26(7):736-743.
Anecdotal observations by Drs. JK and Wendy Winckelbach.




Great article, Bill !!
J
Thanks, J. Where are you?
What is your question?
What question?
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. [Link deleted]
Thank you