HIP FRACTURE
A fracture of the hip is one of the more unfortunate accompaniments of old age. It is a devastating circumstance that alters the lifestyle, mobility, comfort, and life expectancy of the individual who suffers the injury. After hip fracture, most patients do not return to their pre-fracture level of physical and mental performance. Factors such as mental, physical, and nutritional status, co-morbidities, length of hospital stay, post-operative pain and complications all play a role in determining this outcome. An example would be the 90 year old (age), woman (gender), with congestive heart failure (co-morbidity), who is frail (nutrition), and nearly bedfast (physical status) who breaks her hip falling out of bed. Her odds of survival are very low. She very likely will not leave the hospital, but if she does, her chances of long term survival are small.
It is estimated that annually there are 260,000 to 300,000 hospital admissions for hip fractures in the U.S. with 65%-75% of them being in women. The mean age is 79 years, and 86% of hip fractures occur in people over age 65. A fractured hip is a major insult to the entire body causing complications that often result in the patient’s death. In fact, 8%-10% of hip fracture patients die during the first 30 days after and 20%-28% die in the first year after injury. Additionally, complications such as pneumonia, pulmonary emboli (blood clots to the lung), congestive heart failure, urinary tract infections, and septicemia are highly likely to occur post- operatively. These complications occur often in this highly vulnerable population of patients whose physical and metabolic balance is disrupted by a fractured hip.
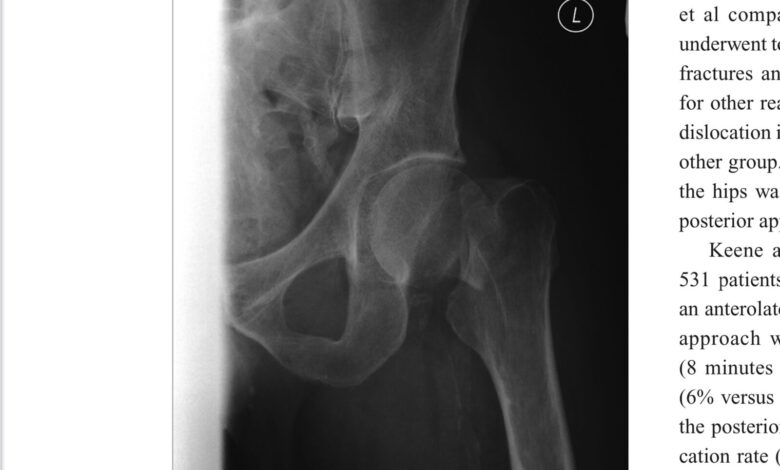
The hip is a classic “ball and socket joint.” It is comprised of two major bones—the pelvis and the femur, or thigh bone. The “socket,” or cup, is in the side of the pelvis at a 45° angle from vertical, and the “ball” is the near end of the femur. The “ball” fits tightly into the “socket” but allows a generous range of motion and flexibility. The socket is called the acetabulum, and the ball is called the femoral head. The femoral head is attached to the long shaft of the femur by a segment called the femoral neck. The attachment of the neck to the femoral shaft is angled downward to accommodate the angle of the socket. Where the neck and the shaft meet the bone is thicker, stronger, and has two bony projections called the trochanters, greater and lesser. Multiple tendons attach to the trochanters to enable the many motions of the hip—flexion, extension, abduction, adduction, internal and external rotation.
The hip joint is held together by a sturdy ligamentous structure called the joint capsule. The hip is then divided into intracapsular and extracapsular halves. Within, or inside, the joint capsule lies the circulatory structures that supply blood to the femur. A fracture involving the intracapsular bone, often cuts off blood supply to the head of the femur causing osteonecrosis, or death of the bone (especially, the femoral head). These fractures often require joint replacement rather than mere fixation with a “nail” or a “plate and screws.”
Hip fractures most often occur in the femoral neck or at the trochanters. There are, however, four common hip fracture sites, named by the fracture location. Anatomically starting from the near end of the femur they are:
1. Sub-capital fracture—the ball (head of the femur) breaks off of the femoral neck at its
attachment.
2. Femoral neck fracture—the neck breaks halfway between the ball and trochanters.
3. Inter-trochanteric fracture—the thick, sturdy area connecting the neck to the shaft breaks.
4. Sub-trochanteric fracture—the beginning of the long shaft of the femur breaks at the
base of the trochanters.
Regardless of location, the injury is serious and requires surgery to stabilize the break and permit early walking. Fall risk increases with age as does the incidence of osteoporosis. These two factors are prominent contributors to hip fractures. An elderly person whose strength and balance are compromised, falls and because he or she has osteoporotic bones, the impact fractures the hip at its weakest point.
If the patient were not operated on to stabilize the break, he/she would have to remain bedfast and not be able to put weight on the fractured hip for months, or until it healed well enough to safely bear weight. During these months, the patient would be subject to everyone of the many complications he/she could experience—pneumonia, pulmonary emboli, urinary tract infection, sepsis, death. Early surgery to stabilize the fracture allows the patient to get out of bed, sit in a chair, and even walk with partial weight-bearing. Early mobilization prevents the many problems that can, and do, occur in an elderly, debilitated patient.
Dr. G’s Opinion: A fractured hip is often “the beginning of the end” for an elderly patient, but it doesn’t have to be. Surgery to stabilize the fracture and permit aggressive and persistent physical therapy is the answer to rehabbing the patient. Purposeful activity prevents the many possible complications and gets the patient going to regain the pre-fracture level of activity.
References: Zhang Y-W, Lu Pan-Pan, et al. Prevalence, Characteristics, and Associated Risk Factors of the Elderly with Hip Fractures: A Cross-Sectional Analysis of NHANES 2005-2010.Clin Interv Aging 2021 Jan 27;16: 177-185.
Alexiou KI, Roushias A, Vartimidis SE, Malizos KN. Quality of life and psychological consequences in elderly patients after hip fracture: a Review. Clinical Interventions in Aging 2018;13:143-150.
Shigemoto K, Sawaguchi T, Higashikawa T, OkuroM. Differences in age-related characteristics among elderly people with hip fractures. J Orthopedic Sci 2023 Sep;28(5):1131-1135.
Collin PG, et al. Hip fractures in the elderly-A clinical Anatomy Review. Clin Anat 2017 Jan;30(1):89-97.
Hayes WC, Myers ER, et al. Etiology and prevention of age-related hip fractures. Bone 1996 Jan;18(1supp):77S-86S
Antapur P, Mahomed N, Gandhi R. Fractures in the elderly: when is hip replacement a necessity? Clinical Interventions in Aging 2011;6:1-7.



Men with hip fractures have a vastly higher one year mortality than women. Osteoporosis in women can be a singular disease, but in men, osteoporosis is associated with severe multi-system issues. Fractures in the subcapital and high neck usually require some type of hip replacement due to the blood supply being severed to the femoral head (vascularity enters at the neck and ascends into the head through the bone).
Thanks, John.