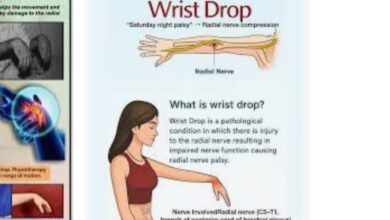
MALLET FINGER
Almost everyone has 8 fingers and 2 thumbs. Thumbs are important but not for this blog. There are 4 fingers on each hand. Each finger has 3 bones, or 3 sections. The bones are called phalanges, or singular, phalanx. Thus, we have a proximal phalanx, middle phalanx, and a distal phalanx. Proximal means nearest the palm, distal means farthest from the palm, and middle means the bone that stands between the other two. The three phalanges are connected by joints called interphalangeal joints (between the phalanges). There is a proximal interphalangeal joint (PIP) and a distal interphalangeal joint (DIP).
Fingers are capable of bending at the joints. Flexion is the name for bending. Extension is the term for straightening of the finger. These two functions are carried out by 3 flexor and 3 extensor tendons. The tendons each attach to the near (proximal) end of each phalanx. The muscles attached to the flexor and extensor tendons are located in the forearm. Thus these tendons are very long and run from the forearm through the palm of the hand, or over the back of the hand, into the fingers.
The tendons of the hand are very strong and very sturdy, and almost never tear or rupture. There is, however, a vulnerable weakness at the end of the tendon where it attaches to a phalanx. This is especially true for the flexor tendon attachment to the distal phalanx. Traumatic injury to the finger will sometimes separate the tendon from the bone. The term for that is avulsion of the tendon. The tendon may simple detach itself from the bone or it may take a fragment of the bone with it. This is called an avulsion fracture.
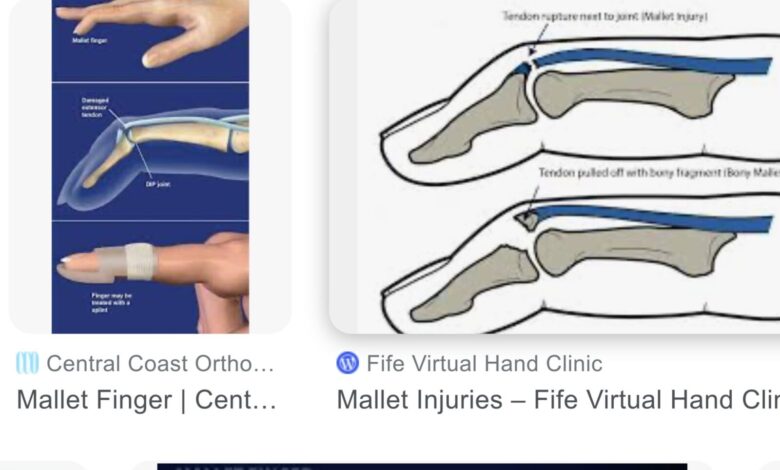
If the flexor tendon avulses, the end of the finger can no longer bend and the finger is straight all the time. If the extensor tendon avulses from the phalanx, the end of the finger cannot be straightened out and is held in a permanent flexed position. Trauma more frequently avulses the extensor tendon from the distal phalanx than the flexor tendon. The permanently flexed distal phalanx is called a mallet finger.
Mallet finger is most common in young males involved in athletic activities or work involving the use of the hands. When a ball, or any hard object, hits the end of a finger with enough force, the distal phalanx gets either bent down (hyperflexion) or back (hyperextension) avulsing the tendon from the bone. By far, the extensor tendon to the distal phalanx is the tendon most often detached, leaving the end of the finger bent downward, thus the term mallet finger evolved. The middle, ring, and fifth (little) fingers, in that order, are affected most frequently.
The diagnosis is easy to make because the finger looks like it does in the picture at the beginning of the post. It’s a classic appearance. Attempts to straighten the finger are impossible because the tendon that performs that function has pulled away from its attachment. Pain, deformity, and loss of function are the criteria needed for a diagnosis. X-rays of the finger are needed to determine if the injury also shows the distal phalanx is fractured or if the extensor tendon has avulsed a fragment of bone when it detached.
The goal of treatment is to restore range of motion of the joint as much as possible and return the function of the distal phalanx. “Non-operative management has been advocated for almost all mallet finger injuries.” This is accomplished by immobilization of the joint by splinting it in a hyperextended position. The hope is the torn end of the tendon will re-attach itself to the bone. Complete immobilization is needed continuously for 6 weeks followed by nighttime splinting for an additional two weeks for this to occur. If reattachment fails, or if function is not restored, another six weeks of immobilization with splinting can be tried, but these and other more complicated cases may require surgical reattachment. Even then, results may not be as hoped.
My experience with this injury was not favorable. The patients I treated did not heal as I would have hoped and were left with a stiff, partially flexed, DIP joint. The extensor tendon did not re-attach itself to the distal phalanx as advertised. In fact, the DIP joint healed (fused), and the patient had a stiff, bent finger. For this to work, the doctor, and especially, the patient need to be diligent and persistent about splinting the joint. Even then, you’re hoping like crazy the torn tendon will reattach to its bony terminus. The splint has to be left in place a full 6 weeks. If healing is not accomplished, another 6 weeks of splinting should be tried. If it isn’t, the mallet deformity will persist forever. And, unfortunately, even in the best of circumstances, in some patients, the deformity will not be altered nor will they regain function.
Successful treatment requires a lot of patience, optimism, and a cooperative patient. One, or all, of those traits were absent in many of the people I attempted to treat. After having limited success with splinting, I came to believe it was better to refer these folks to a hand specialist/surgeon rather than treat it myself. The hand surgeon has the knowledge to know who should have surgery and whether it will help. It is important to treat this injury correctly because long term, it affects use of the affected hand and finger and can be very annoying for the patient. When a mallet finger is treated “successfully,” it will still have a bit of deformity, poor range of motion, or limited function.
Reference: Lamaris GA, Matthew MK. The Diagnosis and Management of Mallet Finger Injuries. Hand 2017;12(3):223-228.
Netscher DT, Pham DT, Staines KG. Finger Injuries in Ball Sports. Hand Clin 2017 Feb;33(1):119-139.