PROSTATITIS

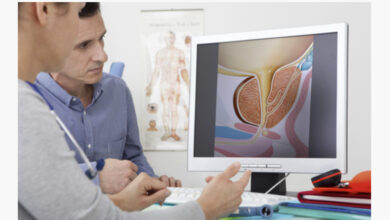
Prostatitis is a disease entity found only in men. The reason, of course, is that only men have a prostate. The prostate is a glandular structure about the size of a walnut that sits at the base of the urinary bladder, and passing through it is the urethra. The function of the prostate gland is to produce fluid and nutrients that provide an environment in which sperm thrive. During sexual intercourse, arousal initiates the production sperm from the testes and fluid from the seminal vesicles and prostate. They mix together to produce seminal fluid, or semen. Ninety percent of semen released during intercourse is fluid from the prostate.
As we age, the prostate frequently enlarges restricting the flow of urine out of the bladder. It continues to produce semen, but over time the volume of fluid lessens.
Very few things can go wrong with the prostate. The biggest worry, obviously, is prostate cancer, the second most common cancer in men (after skin cancer). Of every 100 American men, 13 will have prostate cancer during their lifetime. Benign prostate enlargement is the next concern because of the annoying symptoms it causes as it chokes off the free flow of urine out of the bladder. Lastly, like any part of the human body, the prostate is susceptible to invasion by micro-organisms, ie. it can get infected.
Infection of the prostate is divided into four categories. They are:
1. Acute bacterial prostatitis
2. Chronic bacterial prostatitis (CBP)
3. Chronic non-bacterial prostatitis (CNP)/chronic pelvic pain syndrome (CPPS)
4. Asymptomatic inflammatory prostatitis
Of all cases of prostatitis, only 10% fall into the acute bacterial prostatitis category. Far more common is chronic bacterial prostatitis which presents as recurrent urinary tract infections (UTI’s) with the same organism identified on repeated cultures. If an acute UTI is inadequately treated, symptoms will recur after discontinuation of the antibiotic, causing the situation to be classed as chronic bacterial prostatitis. This is a common scenario.
Acute prostatitis is caused by an “ascending urethral infection.” Any procedure that involves entering the urethral opening in the penis can introduce bacteria. Inserting a catheter into the bladder, cystoscopy, transrectal prostate biopsy, risky sexual behavior, and an uncircumcised penis are examples. Infection elsewhere in the urinary tract (epididymitis, orchitis, urethritis) can spread into the prostate.
Symptoms of prostatitis include frequent urination, burning with urination, the constant urge to urinate, and cloudy urine. Going more often at night is a sign as well. As the infection worsens, pain in the prostate area increases and symptoms such as fever, chills, nausea, and vomiting are possible.
The diagnosis of prostatitis is made using several factors. They are:
The patient’s symptoms are classic for a UTI
A urinalysis which shows cloudy urine with WBC’s, protein, bacteria
Digital rectal exam reveals a swollen and very tender prostate
Urine culture is positive for bacteria that commonly cause prostatitis
The doctor can’t make an accurate diagnosis of prostatitis unless all of the above factors are present. The doctor can diagnose a UTI by history and urinalysis, but unless a tender prostate is found on rectal exam, he/she can’t say the patient has prostatitis. Often a lot of latitude is given to these criteria, but to be certain of the diagnosis, they should all be present. A large percentage of prostatitis patient fall into the chronic bacterial prostatitis category because their initial treatment was not long enough or not the most effective antibiotic. Vigilance by the treating physician can avoid this outcome.
All cases of Prostatitis are treated with antibiotics. The majority can be treated adequately with oral antibiotics. Numerous drugs or drug combinations can be used, but that decision should be made based on the results of a urine culture and drug sensitivity testing of the organism found on culture. Prostatitis requires longer duration of therapy than does a simple case of female cystitis. Regimens lasting 10-14 days for mild infections and 4-6 weeks for severe infections are used. Febrile patients or patients at risk of sepsis should be hospitalized and given intravenous antibiotics.
Dr. G’s Opinion: Infections of the urinary tract, especially the male urinary tract, should never be taken lightly. The potential for chronic infection and progression to urosepsis (infection in the bloodstream) are big concerns. Treatment regimens need to be completed by the patient. A follow up urinalysis and urine culture should be done to confirm the infection is completely gone. If it isn’t gone, or recurs within a short time, a referral to a urologist for evaluation should be done.
References: Coker TJ, Dierfeldt DM. Acute Bacterial Prostatitis: Diagnosis and Management Am Fam Phys 2016 January 15;93(2):114-120.
Magritte V, et al. Multidisciplinary approach to prostatitis Arch Ital Urol Androl. 2019 Jan 18;90(4):227-248.
Holt JD, Garrett WA, McCurry TK. Common Questions about Chronic Prostatitis Am Fam Phys
2016 Feb 15;93(4):290-296.
Brede CM, Shoskes DA The etiology and management of acute prostatitis Nature Reviews Urology 2011 March 15;8:207-212.