HEART ATTACKS IN WOMEN: Are They Really Different?

For many years, the mantra has been that heart attacks in women are different; they are harder to diagnose, the symptoms are vague and different, and they are missed 78% of the time. Alarmingly, the chance of a fatal outcome is greater, too. Why is that? Numerous studies have been conducted to investigate the reasons.
Heart disease is the leading cause of death in both men and women, and one-third of women have some form of cardiovascular disease. The average age at which women have their first heart attack is 72 and for men it’s 65. Since 1984, the death rate from heart disease in women has been increasing, and each year, more women than men have died from heart attacks.
Some reasons for the difference in heart disease are physiologic and behavioral. Women have anatomically smaller hearts and faster heart rates, and when stressed, the heart beats faster and pumps more blood. Men smoke and drink more than women, tend to be less healthy, and have more stressful jobs. Before you accuse me of sexism, I must also state that since the 1980’s, as more women entered the workforce, their rate of heart attacks increased.
There is, however, a degree of sexism in the diagnosis of heart disease. When a man comes to the ER with chest pain, doctors think he’s had a heart attack until proven otherwise. Women, on the other hand, under the same circumstances, are thought to be anxious until proven otherwise. There is “gender bias” in play that leads to the worrisome statistic than 78% of heart attacks in women are missed.
Women have symptoms that aren’t always the classic “crushing chest pain, radiating to the left arm, accompanied by sweating and weakness!” Instead their symptoms are somewhat atypical and under-appreciated. Yes, women have chest pain, but more frequently complain of nausea, dizziness, and fatigue, all symptoms of low cardiac output. Shortness of breath, back, neck, and jaw pain are common, too. Because of these vagaries, women delay seeking medical care for 54 hours while men are in the ER in 16 hours.
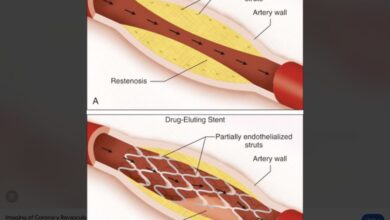
The process of forming a blocked coronary artery (a plaque) occurs exactly the same way in men and women, as you would expect. But as mentioned above, women have their first heart attack 7 years later in life than men, and shockingly, 47% of women, and 36% of men, die from their first attack. That difference is attributable to a delay in diagnosis because of the atypical symptoms women experience. When a woman presents to the ER, unless she has obvious EKG changes or is in shock, more than three-fourths of the time she may be diagnosed with something else.
The effort to train physicians to be hyper-aware of heart disease in women has been ongoing for several years. Male physicians, in particular, need to erase from their minds the notion of “the weaker sex,” and realize women are just as likely, if not more so, to have real disease caused by the stresses of life. The phrase “a woman’s work is never done” is very true. There’s always something or someone to take care of so their responsibilities and stresses are endless. Men come home, sit, watch TV, nap, are waited on, and have several hours of down time. Men are expected to have heart attacks because of unhealthy lifestyle choices. Women aren’t expected to have heart attacks and don’t receive the same attention as men because of this different perspective.
Early last year, a female friend had a classic example of just what this blog is all about. For many years she had been bothered by heartburn and acid reflux symptoms. The drug she took for the symptoms was taken off the market and substituted with famotidine. About that time she had a flare-up of heartburn and indigestion that she attributed to the medication change. She found herself doubling the dosage of famotidine and taking Tums more than usual, especially at night, when the symptoms were worse. Still thinking this was acid reflux, she continued to take walks and do yoga without the symptoms worsening until early one morning when new symptoms appeared. She had not previously had heartburn in the morning, and that concerned her. Nor had it been accompanied by nausea or sweating. But when all of her fingertips became numb and tingly, she knew something else was going on. At this time, her “heartburn” perception was replaced by “pain” she described as 7 of 10 in severity. During this episode, she never had jaw, neck, or arm pain as is so common.
She was later found to have had a heart attack and several blockages that were angioplastied and stented. The best part of this scenario was the response she received from her primary care doctor’s office that morning. The person she spoke to was perceptive enough to realize her symptoms could be of cardiac origin and initiated an evaluation that probably saved her life.
This and countless other scenarios are typical of the odd manner in which women present with coronary artery disease and heart attacks. Healthcare providers need to discard their notion of the classic presentation of a heart attack in women. If the patient is female, assume any “pain” above the abdomen is of cardiac origin until you have proof of another cause.
References: Westerman S, Wenger NK. Women and heart disease, the underrecognized burden: sex differences, biases, and unmet clinical and research challenges. Clin Sci (Lond) 2016 Apr;130(8):551-563.
HTTPS://www.cdc.gov/heart disease/women
HTTPS://www.cedars-Sinai.org/newsroom/time-women-die-from-heart-attacks-more-often-than-men-here’s-why-and-what-doctors-are-doing-about-it.
HTTPS://www.texasheart.org/heart-health/heart-information-center/topics/women-and-heart-disease.
2013 American Heart Association Statistical Fact Sheet “Women & Cardiovascular Diseases
HTTPS://www.clevelandclinic.org/women-men-higher-risk-heart-attack
Varga L. Don’t miss a beat. Know the signs of a heart attack in women. Costco Connection 2021 Feb:73.