HYALURONIC ACID
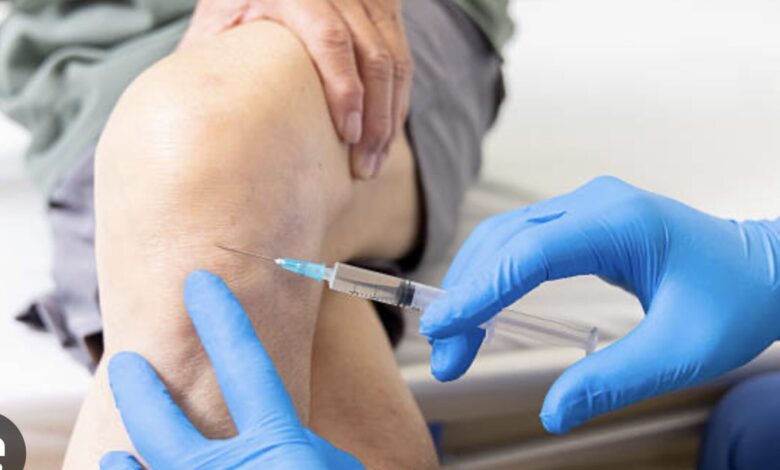
Hyaluronic acid is the main ingredient in all those products that rheumatologists and orthopedic surgeons inject into the knees of patients suffering from severe degenerative arthritis. The purpose of the injections is to produce a protective coating over the bony surface of the joint that replaces the eroded cartilage, “lubricate,” or moisten the joint, and relieve the pain that severely limits walking. Hyaluronic acid is a natural substance produced by the body, and is actually a complex molecule composed of simple sugars bound together. It’s called a polysaccharide.
Hyaluronic acid, itself, is not the actual substance used in these products. Instead, it is altered chemically to adapt it to the use for which it is intended. It is found in several other products that are oral, over-the-counter pills or liquids or topical lotions, creams, ointments, gels, or shampoos. It is a frequently used compound. I have little first hand experience with Hyaluronic acid used for other than for relief of arthritis pain, and my experience with it for arthritis is all from patients’ comments. I did not inject it into joints for the temporary relief of pain. My opinion of Hyaluronic acid is based totally on reports from patients who received injections most often in the knees.
What I have observed from patient reports is mostly negative. In the majority of cases, patients receiving intraarticular injections of Hyaluronic acid have “end-stage” osteoarthritis and are having the injections to delay having knee replacement surgery. Thus their arthritis is severe and the chances of these injections helping are small. They get temporary relief of six months or less duration and eventually need surgery.
The number of patients who said they got significant long term relief from injections of Hyaluronic acid preparations can be counted on one hand. My suspicion is that these patients had arthritis that was symptomatic but not bad enough just yet to send them to the operating room. In these folks, the Hyaluronic acid preparation was successful in protecting the cartilage and delaying its further deterioration.
The recommendation for Hyaluronic acid injections is for “mild to moderate osteoarthritis.” In these patients, a 60% to 70% success rate for up to six months is reported, and a 50% reduction in pain is an expected outcome. As previously mentioned, however, my experience has not been that good because the patients selected for injection had severe osteoarthritis that responded poorly to the preparation. Had my patients been injected earlier in their disease, their results would probably have been better.
For the oral, topical and OTC preparations containing Hyaluronic acid, the FDA has recently issued an advisory warning about the use of several non-prescription products that contained ingredients not listed on the label. These ingredients were dexamethasone (a high potency corticosteroid) and diclofenac (a powerful NSAID) that were said to pose “serious risk to your health….and can lead to severe health issues.” The products were named and consumers were warned not to use them.
Would Dr. G ever have intra-articular Hyaluronic acid injections? I don’t know, but probably not. I’ve had cortisone injections several times. They help almost immediately, but don’t ease symptoms for more than 3-6 weeks. Also, Corticosteroids are known to harm the surface layer of cartilage in the joints, so while they relieve pain, they also worsen the underlying condition.
My opinion of Hyaluronic acid joint injections is negative because of reasons mentioned above. I admit bias when considering these injections, but it’s based on using it in the wrong group of patients.
References: www.google.com/my.clevelandclinic.org/viewarticle/hyaluronic-acid
Collins TR. FDA to Consumers: Don’t Use These Hyaluronic Acid Products Medscape 2026 April 10.
www.google.com/synvisc.com



My family has had 2 hyaluronic knee injections for moderate osteoarthritis. Not one bit of improvement.
My experience, too.