SHINGLES VACCINES: Do They Work?
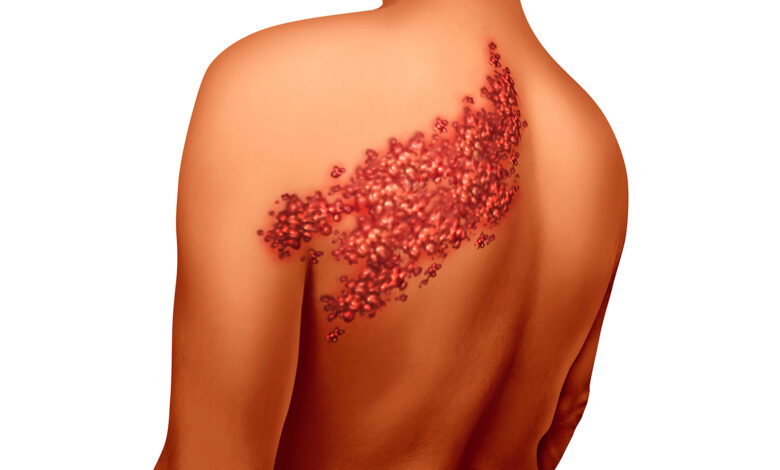
Herpes Zoster, aka Shingles, is a disease human beings find quite unpleasant. Because it falls in the Herpesvirus classification, it gets equated with genital herpes and fever blisters, and, thus is sometimes stigmatized. Chickenpox, or Varicella, is another disease caused by a Herpesvirus, but since the majority of chickenpox cases occur in innocent children, it’s considered part of growing up.
Chickenpox (Varicella) is caused by the Varicella-zoster virus. After a bout of chickenpox, for unknown reasons, the virus lies dormant for many years in the nerve root structures next to the spine until still-undetermined factors cause it to travel along the nerve to the skin. When the virus reaches the skin surface, the area supplied by the nerve (a dermatome) breaks out with the painful blisters of shingles.
Occasionally, patients will have an annoying, aggravating pain for as long as two weeks before the blistery rash develops. That poses a real dilemma for the patient and physician—the patient has severe pain and the physician cannot find a clear-cut cause until the rash appears. Then, it’s obvious what’s going on.
When shingles “heals,” the blisters dry up and scab over. Visible remnants (scars) sometimes remain, but of more concern is the painful neuralgia that occurs in as many as 20% of shingles cases. Eighty-five percent of Postherpetic Neuralgia patients are over 50 years old, so this debilitating disorder occurs in vulnerable individuals.
Just as our recent experience with COVID-19 tells us, vaccines are imperative to put a stop to shingles, or at least to lessen its severity. Shingles isn’t considered a fatal disease, but when the pain of postherpetic neuralgia is severe, as it frequently is, some people wish they would die. In fact, there have been suicides by patients who had postherpetic neuralgia of the scalp or face.
There wasn’t any Operation Warp Speed in effect for the development of shingles vaccines so it took a long time for them to make it to “market.” Merck was first in 2006 with Zostavax and Glaxo Smith Kline (GSK) presented Shingrix in 2017. They are very different vaccines with significantly different efficacy rates. Zostavax is a single shot while Shingrix requires two shots 2-6 months apart.
Zostavax is a “live-attenuated” vaccine meaning it is an altered version of the Varicella-zoster virus which, when injected into humans, stimulates the immune system to produce antibodies against the virus and thus prevent shingles. Unfortunately, it was effective only 70% of the time, and over an 8-year period efficacy drops from 68.7% to 4.2%. That means that 6-8 years after vaccination you are no longer protected from getting shingles. This was an unacceptable result so Zostavax has fallen out of favor. Also, it was only 67% effective in preventing post-herpetic neuralgia, and that immunity wanes, too.
Shingrix is a “non-live, subunit vaccine” that works by introducing “only an essential subunit of the actual virus.” That sounds complicated, but what it means is this vaccine’s delivery system produces much better results in preventing shingles without using a live virus. Studies showed Shingrix was 97% effective against shingles for people between the ages of 50 and 69 and 91% effective for people 70 or older. The clinical trials included over 38,000 participants, a large sampling of patients. Shingrix was also 91% effective in preventing PHN in patients 50 and older, and it remains 85% effective for up to 4 years after vaccination. As time passes immunity wanes, but not as rapidly or as significantly as it does with Zostavax.
I received both shots; Zostavax, in 2008 and Shingrix in 2019. In late 2020 I was shocked when I developed shingles in the C7, C8, and T1 dermatomes of my right upper extremity. I take two immunosuppressive drugs so despite having an extensive rash, I didn’t have much pain. The immune system drugs I take caused me to have a weak response to the vaccines. I still got the rash, but the pain was not intolerable. Having the shots (all 3) yet still having shingles was a bit of a surprise and places me in the outlier/enigma category. Even though I was vaccinated against it, I got shingles! Fortunately, I did not get postherpetic neuralgia. The vaccines worked at least that well.
Dr. G’s Opinion: The CDC recommends two doses of Shingrix given 2-6 months apart injected in the deltoid muscle of the upper arm. Shingrix clearly has significantly better efficacy than Zostavax and should be the vaccine of choice. It is recommended for anyone age 50 and over, even if they’ve had shingles or previously received Zostavax. It costs a bit more than Zostavax and is usually not covered by insurance, but Medicare Part D plans often do cover it. Vaccine safety has been well-established and should not a deter a patient from receiving the vaccine.
I would recommend making an appointment with your doctor or pharmacist to get the Shingrix vaccine shots ASAP. Right now you only need two shots 2-6 months apart. When you get Shingrix vaccine, a COVID-19 booster, and an annual flu shot, you will be all set for winter.
References: Singh G, Song S, Choi, E, Lee P, Nahum FS. Recombinant zoster vaccine: a new option for the prevention of herpes zoster and post herpetic neuralgia. Korean Pain J 2020;33(3):201-207.
“Shingles Vaccines: Do they work?” DrGOpines.com 2018 June 20.—78 (9/4/2021).