TOP 10 RISK FACTORS FOR PANCREATIC CANCER
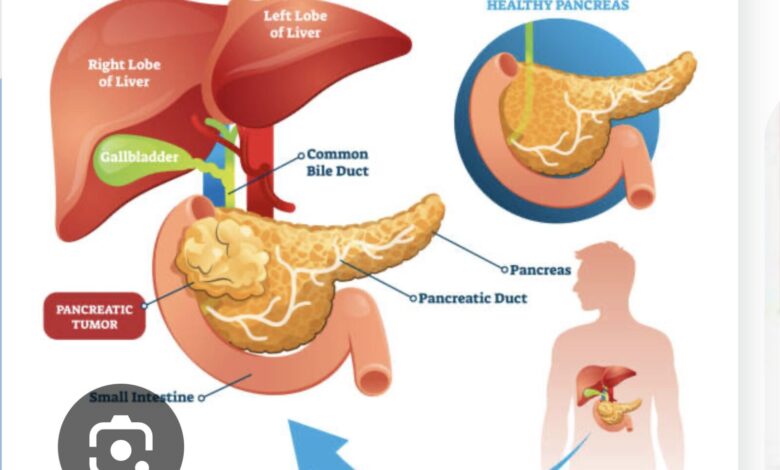
In the last five years, I have personally known five people who died of cancer of the pancreas. In 1968, my father died of this horrible disease at the age of 55. Medical and hospital care were different in 1968 because he was admitted to Community East in mid July and was allowed to stay in the hospital until his death October 1. Pancreatic cancer was not common back then, possibly because technologies to diagnose it, like CT scans, MRI’s, and ERCP’s, did not exist. Most cases were like his: diagnosed at the time of an abdominal surgery (a laparotomy) done because the doctors did not know what was wrong with him. He was found to have carcinoma (cancer) of the head of the pancreas, obstructing his common bile duct, causing jaundice and widespread liver metastases.
The reference for this blog stated the incidence of pancreatic CA has doubled in the past 20 years. The ability to diagnose pancreatic cancer has improved, but the prognosis after diagnosis is still dismal. Five year survival rates have improved, but need to be better. In 1968, a 5-year survival of 5% would have been overly optimistic. In 2015, it was just below 7%, but last year, 2025, it doubled to 13%. That’s probably because of earlier diagnosis and better treatment.
However, prevention and elimination of the risk factors that can be eliminated are still best. This article talks about 10 risk factors that researchers continually report as significant in diagnosing and treating CA of the pancreas. They are:
SMOKING: One of the worst carcinogens ever contrived. Smokers are nearly twice as likely to develop pancreatic cancer (my dad smoked Lucky Strikes). Cessation lowers the incidence over time, and “the risk approaches that of never smokers.”
ALCOHOL CONSUMPTION: More than 3 drinks a day has been associated with an increased risk for pancreatic CA. My dad was a 2 beers a day drinker.
HIGH BMI (obesity): A BMI Above 30 is an independent risk factor for pancreatic CA. My Dad was heavy but not obese.
DIABETES: New onset diabetes or sudden worsening of glycemic control can be an indicator of the presence of pancreatic CA.
DIET: Red meat and more than 2 sugary beverages per day increase one’s risk for pancreatic cancer. A diet of plant-based foods, nuts, and Mediterranean style cooking reduce risk.
PANCREATITIS: “Can be both a cause and a consequence of pancreatic cancer….The risk is particularly elevated within the first year after an episode of pancreatitis.”
AGE: Risk increases after age 40. 80% of cases occurred between ages of 60 and 80.
FAMILY HISTORY OF PANCREATIC CANCER: Close family relatives should undergo a screening MRI of the bile ducts and pancreas.
GENETIC PREDISPOSITION: If you have a cancer gene, you’re at higher risk of pancreatic CA.
PREMALIGNANT PANCREATIC LESIONS: Certain lesions of the pancreas are considered pre-malignant and may progress to cancer. When they are discovered they should be removed.
Dr. G’s Opinion: Pancreatic cancer may be the worst cancer out there. Being pro-active and diagnosing it early is very important for a good outcome. If those risk factors, especially family history, are present, do whatever is necessary to get diagnostic screening tests done.
Reference: Kim GE. Pancreatic Cancer: Top 10 Triggers for an Often-Silent Disease. Medscape 2026 February 13.